Co-design of pathway and manual for a dietitian-led approach to the management of type 2 diabetes in Nepal

Characteristics of the participants
A total of 19 service users, health service providers, and other stakeholders were involved in different events during the design and evaluation of the diabetic education manual (Table 1). Four patients with T2D, two family caregivers, two general physicians, two consultant physicians, two paramedics, two nurses, two dietitians and three public health professionals were involved in the consultative meetings. Likewise, three patients with T2D who have been on medication for 3 to 5 years, two family caregivers, a paramedic, a nurse, two dietitians, and two public health professionals were involved in the co-design workshop. A total of nine participants from diverse backgrounds were interviewed to explore the feasibility and acceptability of the manual.
Co-design workshop
The results from the co-design workshop have been presented one by one, organised by specific sessions under corresponding thematic headings.
First session: discussion on issues in the management of diabetes
In the first session, the research team initiated the discussion by presenting a brief overview of the literature on T2D management issues in the Nepalese context to facilitate a detailed discussion. The discussion highlighted a lack of diabetes patients’ knowledge about healthy diets and physical activity, medication initiation and adherence, confusion about blood glucose monitoring tests, and harmful socio-cultural belief systems, which were individual-level barriers to self-management of T2D. Likewise, inadequate counselling, a lack of guidelines and protocols for treatment and counselling, and dietary guidelines for patients with T2D were some of the challenges on the provider’s side in managing T2D. Furthermore, there was an in-depth discussion on practical healthcare system issues and other challenges in the management of T2D. The discussion was summarised under four key thematic headings, such as complexities of diabetes management, social and behavioural challenges, dietary recommendation and adherence challenges, and service provider responses and treatment approaches (Table 2).
Second session: discuss the solutions for the dietary approach in diabetes management
In the second session, two key components were discussed and finalised: first, the pathways for a dietary approach to managing T2D were extensively discussed and drafted. Secondly, the contents of the nutrition education manual for patients with T2D were discussed and agreed upon.
Pathway for a dietitian-led dietary approach for the management of T2D
This pathway illustrates the channel for treating and managing T2D through a dietitian-led dietary approach (Fig. 3). The first step in Fig. 3 shows that individuals in the community at risk of T2D or patients with T2D seek health services at their preferred health facility. In the second step, individuals visit the health facility for an initial diagnosis and confirmation of T2D, either through a community screening program or self-referral. At the same time, the patient, who had previously been diagnosed with T2D, also sought similar health services at their preferred health facilities. Nepal’s healthcare system has primary, secondary, and tertiary health facilities. The potential patient is expected to visit a general physician (GP)/consultant for a check-up at any of these health facilities. In the third step, the patient will be referred for blood tests to confirm T2D status. Again, the patient is expected to visit the GP for further consultation after receiving the blood report. A physician/consultant is supposed to refer patients with T2D to a dietitian for appropriate nutrition counselling and a diet plan after completing the consultation at their clinic. In the fourth step, the trained dietitian will then provide essential nutrition counselling to the patient and their caregiver following the nutrition education manual. The dietitian will also provide the patient with a copy of the nutrition education manual and a scheduled individualised diet plan sheet in their local language. In the fifth step, the patient visits the pharmacy to get prescribed medications. Finally, the patient will return home after receiving specialised nutrition counselling and a diet plan, plus prescribed medications. The patient is expected to adhere to the clinician’s prescriptions and the dietitian’s menu plan. Furthermore, the patient is expected to visit their consultant regularly, every three months, and undergo a blood test to check if their fasting blood glucose and HbA1c levels have decreased. This concept was designed based on a patient-centred care approach, which means advocating the needs, preferences, values, and active involvement of patients at the centre, with respect, compassion, and coordinated care and treatment [26].
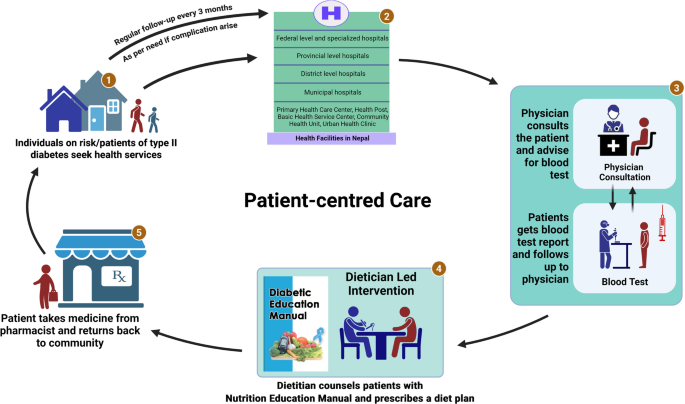
Pathway for dietitian-led approach to the management of T2D
Contents of nutrition education manual for T2D management
The data from the workshop identified the contents of the nutrition education manual for T2D. The manual’s contents were designed with the understanding that the patient may not have prior knowledge about T2D. The contents of the nutrition education manual are summarised in the table (Table 3).
The key emphasis throughout the workshop discussion was to use simple language and minimise the use of technical terms in the nutrition education manual whenever possible. Metaphors in diagrammatic form were used to illustrate the pathway of insulin-regulating blood sugar levels in the human body, allowing patients without prior knowledge of T2D to easily understand the educational content (Supplementary file 1). Despite the wider consensus on including the comprehensive aspects of the educational content for managing T2D, the nutritional components were discussed more, and it was agreed to present the nutrition-related information relating to local availability of food choices and patients’ socio-cultural behaviour. The specific suggestions provided for the inclusion of nutrition aspects were focused on the importance of a healthy diet for people with T2D, dietary recommendations for people with diabetes, selection/choices of foods for controlling and managing diabetes, and key information to be considered while selecting quality fat. Further, the discussion also highlighted the local contextual issues related to food choices which need to be included in the manual, such as additional food items recommended while hungry, healthy food selection and cooking techniques, choices of foods while attending social events by diabetic patients and lifestyle management. The food choices, considering the local socio-cultural and behavioural context, have been included in the table format as a food exchange list for patients with T2D (Supplementary file 1).
The simple colour-coded chart was developed to illustrate the different types of diets for patients with T2D: foods that can be normally consumed (green colour), foods that can be occasionally consumed in small amounts (yellow colour), and foods that should be prohibited (red colour) (Supplementary file 1). Similarly, the concept of “My Plate” has been placed at the end of the manual (Supplementary file 1). The picture of “My Plate” is expected to help the patient relate their individualised diet plan with the food items/categories acceptable to consume at different time intervals in their daily food intake.
Validation of the nutrition education manual contents
Acceptability
The results of the qualitative interviews showed that most participants, including service users (patients with T2D), dietitians, physicians, and public health experts, highly acknowledged the contents and design of the manual. They highlighted that the manual could be valued not only by patients with T2D but also by their family members and carers, who should also know the importance of a dietary approach to managing T2D. One of the patients with T2D reflected on the overall contents and colour-coded presentation of the manual contents:
“…this booklet (manual) has adequate information not only for patients but also for their family members…I found adequate information regarding diabetes mellitus and its types, as well as treatment options and tips for a healthy lifestyle and consuming a quality diet. There are pictures and information alongside, so I can remember many things from it… there are different colours in the food exchange chart, which is very informative and practical to understand… Most importantly, there is a diet plan at the end, which is very important for the management of T2D.” (Patient with T2D).
Similarly, the food exchange list presented, considering the Nepalese socio-cultural and behavioural, as well as the availability of food items, was widely accepted by both experts and patients. One of the dietitians commented on the contents of the manual, referring to the food exchange list as:
“I appreciate the local food exchange list because there are taboos regarding food for diabetic patients in our society, and the patients even sometimes fall into depression as they have the same monotonous diet…here the local food exchange list can help a lot to have changes in the choices of food to be consumed. For example, many patients avoid fruits or say they eat the same fruit every day, and they come to us and ask if they could change the fruit they eat. We can show them this manual and teach them what and how much fruit to consume. In addition to this, ‘My plate’ is an effective infographic for patients as they can easily remember it.” (Dietitian).
Another dietitian spoke on the issue of manual content and its relevancy in counselling patients with T2D:
“…the contents in the manual are enough to step up the counselling context for patients with T2D… this manual is kind of the basic guidelines for dietitians as well as patients, which is not available to date…” (Dietitian).
Likewise, physicians and endocrinologist also expressed their acceptance towards the contents and their importance in the behaviour change of patients with T2D. One of the highly experienced consultant physicians remarked.
“…the diabetic education manual would be a great initiative to manage diabetes s… the contents in the manual are highly relevant and practical… what a doctor or Dietitian might forget to explain during the patient’s visits can be easily referred to in this manual so it will help like a checklist for service provider and as well as patients can read it themselves… Not only patients but also other family members who have no prior knowledge of T2D can understand this manual. The manual also has medical nutrition therapy, which is helpful for dietitians, physicians, patients, students, and laypersons.” (Consultant Physician).
Another service provider also confirmed the validity of the contents in the manual and mentioned that:
“…patients can grasp the information through the infographics kept in the manual…Colour codes are genuinely used here to mark important topics, as well as the food exchange charts and other ‘dos and don’ts’ sections. The manual is both handy and portable in terms of size. I also like the paper and colour quality here…. Additionally, it is equally important to assess how effectively the patient is receiving the shared information, so the dietitian can encourage the patient to return for follow-up appointments and reinforce the information.” (General Physician).
In addition, all participants, including the patients with T2D, public health experts, nurses, GPs, and consultant physicians, acknowledged the manual’s contents. One expert who has long experience working in the design, development, and implementation of behavioural change programs commented on the manual.
“The manual is well-designed, and the pictures are relevant in places and easily understood by all levels of readers. Maybe the content, like the introduction, is a bit lengthy, but they are, after all, important to the readers, so that’s fine, too…there are nutrition facts like what and how much to eat, acceptable diets, and these can help the patients to stay healthy so these can be acceptable among patients…can be a practical approach to behaviour change among patient with T2D if implemented effectively…”(Public Health Expert).
Feasibility
The results from the interviews showed that the participants’ confidence in understanding the contents of the manual, the use of local language, and the use of colour-coded pictures to illustrate food choices and portions for patients with T2D were repeatedly reflected as favourable factors for the effective implementation of the manual. It was perceived that the contents in the manual were more likely to be accepted among users due to their simplicity and practicality. The participants also considered that the manual could bridge the gap between the clinical and dietary approaches to managing diabetes and support the integrated management of T2D. Further, the manual could guide patients with T2D in modifying their diet and health-related behaviours practically.
One of the highly experienced Consultant Physicians commented on the practicality of the manual:
“This manual is essential for the integrated management of diabetes. I view this manual development and dietitian counselling as an essential step in the behaviour change of patients with T2D… They will accept the information in the manual and try to follow accordingly to change or upgrade their health status, but continuity is what takes more sacrifice and dedication. They have to continue the treatment measures provided in the manual; they have to adhere to lifestyle modification strategies and care for their diet..concept of ‘My Plate’ at the end, I guess the patient would like it, and also, it will be very easy for us and the dietitian to explain how a food plate should look like and can be followed…” (Consultant Physician).
Likewise, the dietitians believed that the manual could be a practical guideline for counselling patients with T2D. They also believe that this document could save them time in educating patients with diabetes during counselling on dietary approaches to managing T2D. This will further help to improve the patient’s outcomes sustainably. Views of the dietitians reflected on the feasibility aspects of the manual:
“…this manual can help us with counselling guidelines, and as a checklist so we don’t forget what should be included while counselling the patient with T2D….We often forget to mention hypoglycaemia. Even doctors forget it while counselling, which has even led to the death of patients… This will obviously help in managing hypoglycemia….The colourfulness of ‘My plate’ is very effective, which could be effective for even illiterate patients during counselling…” (Dietitian).
“The Nepali language used in the manual can be easily understood; however, some medical terms need to be clarified to the patients during counselling…” (Dietitian).
Further, the design and contextual contents of the manual were believed to be crucial for its adaptation among a wider range of patients with diabetes. One of the patients with T2D expressed his views about the manual:
“There are a lot of things which is of great importance to a patient with diabetes. Even many patients like me who have faced diabetes for a long time learned new information from it…The size of the manual is handy, and the paper quality is also good; it is unlikely to get damaged. Many patients can learn various essential things from this comprehensive and easy-to-understand manual. After going through this manual, now I am able to manage my hypoglycaemia…I will for sure use the manual as it is very informative for me…” (Patient with T2D).
In addition, other stakeholders, including public health experts, provided their positive views regarding the adaptability and implementation aspects of the manual. However, few stakeholders highlighted the time restriction among dietitians due to an inadequate number of experts in the hospital and a high number of patients followed in government hospitals, which could make it difficult to implement the complete contents of the manual due to counselling. Also, it was highlighted that dietitians need to have training before implementing the manual to have adequate information regarding the manual so that they can easily summarise it to the patient in a practical manner within a very short time. There needs to be an allocation of relatively more time for illiterate patients so they can understand the contents explicitly, and regular follow-up should be arranged, especially for those illiterate patients, to adhere to the manual sufficiently. One of the public health experts commented that:
“If the dietitian can provide about 30 minutes during counselling, that would be very effective. However, if only 5–15 minutes is provided, it would be only surface information. The feasibility of practising a diabetic education manual will depend on how much time a dietitian can provide for counselling; there might be a patient flow factor…. patients need to be followed up, and they must be made aware of the improvement in diabetes management that has happened to them due to adherence to the manual. As people have their own ethnic/cultural and religious backgrounds, it may not always be possible to accept the information provided in the manual, but continuous follow-up and awareness that this information can help enhance the usability of the diabetic education manual for patients.” (Public Health Expert).
Another participant was also highlighted by one of the dietitian practitioners, who showed doubt in delivering the complete manual content during the limited time for counselling:
“It’s time-consuming if we go through the topics one by one. It would be difficult to cover all the contents as patients have less time for counselling.” (Dietitian).
Similarly, the colour-coded contents in the manual, related to traffic lights, the concept of “my plate” in relation to the diet plan, and food portions in the manual, were perceived as a convincing way to communicate messages to patients about their dietary management. One of the nursing personnel noted that:
“Often, we listen to the information from health workers but forget it, but with this manual, it will be easy to catch and learn with pictures and traffic light colour codes. I also explained the plate mainly as a dietitian. The current counselling practices related to food choices and portion size are confusing, but this manual clearly presents the food choices and portion size with the example of “my plate” and will make it efficacious for the patient.” (Nurse).
Furthermore, health service providers believed that the manual could enhance the quality of care and effectively improve the delivery of health services among patients with T2D. They also mentioned that patients will understand the healthcare system well and benefit from the integrated health services. This could also improve the effectiveness of counselling services and the demand for qualified dietitians in the hospital, where dietitians often lack the ability to deliver counselling services to patients.
“It is easy for patients with all the information, including an introduction, regular check-ups, causes, dangers, diet menu, food exchange list… This will give broader ideas that are difficult to gain from another authentic source. The manual will facilitate the effective development of health services among patients with diabetes.” (General Physician).
link





