Training clinicians to facilitate diabetes group visits | BMC Medical Education

Setting
Trainings occurred at two nonprofit community clinics in Houston, Texas. Each site hosted a separate training, totaling two trainings. The clinics served uninsured individuals who were primarily Hispanics (> 80%) and largely undocumented immigrants (> 50%). Each site expressed an interest in improving type 2 diabetes care through group visits but did not have established programs.
Eligibility, human ethics, and consent to participate
Learners were required to be clinicians licensed to prescribe medical therapies with a foundational medical knowledge of type 2 diabetes, demonstrated by an active credentialing status at their respective clinic and seeing patients with type 2 diabetes in their practice. Learners were not paid during training; they would be paid if they participated in subsequent group visits. Facilitators conducting the educational sessions for clinicians were primary care physicians with at least five years of experience, who were active in clinical care, and who had prior experience conducting group visits in low-income settings.
This study is part of a larger clinical trial evaluating the use of telementoring to support clinic teams—including clinicians and Community Health Workers—in implementing diabetes programs for uninsured, low-income Hispanic participants (#NCT04835493). Using a consent form, study participants provide their informed consent to participate in the research. This work was conducted in accordance with relevant guidelines, such as the Declaration of Helsinki and approved by the Baylor College of Medicine and University of Texas Medical Branch Institutional Review Boards (IRBs) #49,672 and #22–0224, respectively.
Research design and data analyses
Curriculum planning and development
We used the Analysis, Design, Development, Implementation, Evaluation (ADDIE) model as a theoretical and practical framework to design and develop the curriculum and training (Fig. 1) [10]. With roots in military practices, the ADDIE model provides clear instructional steps, enabling subsequent adoption for medical curricula, and remains a key mechanism for organizing educational content decades after its inception [10]. The current curriculum includes a comprehensive approach to diabetes, including education on testing, dietary interventions, exercise/activity programs, and medications, to enable learners to deliver effective and personalized patient care.
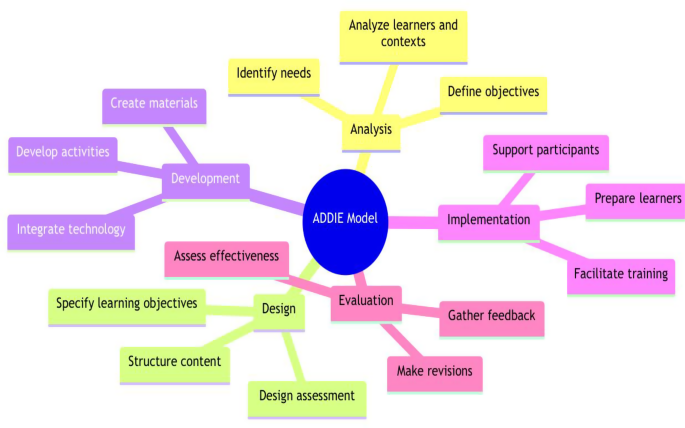
A conceptual diagram of the use of the ADDIE model (Analyze, Design, Develop, Implement, and Evaluate) for clinician learners participating in diabetes group visit training
Analysis step
In the Analysis Step, we outlined the instructional goal and its objectives. We aimed to teach learners how to facilitate group visits by accomplishing the following objectives: (1) outline the logistics of facilitating a multidimensional diabetes group visit program, (2) utilize medication algorithms designed for populations with low-income to determine diabetes, hypertension, and hyperlipidemia pharmacotherapy for patient encounters, and (3) develop plans to address socioeconomic, cultural, and access to care barriers in underserved populations through case studies and role-playing. To address limitations in time and provide flexibility, we chose to conduct the training virtually and held training sessions after work hours [11].
Design step
In the Design Step, we developed the training’s content. We used evidenced-based literature, including guidelines from the American Diabetes Association, American Association of Clinical Endocrinology, Eighth Joint National Commission, and the US Preventive Task Force [12,13,14,15]. The training was divided into two main sections: group visit facilitation and patient encounters. We created a slide presentation to include the training content and added items to enhance learner motivation, such as an ice breaker question at the beginning, case studies, a question/answer section at the end of the training, and 10-minute breaks in between each section.
Developmental step
The Developmental Step provided content to the training. For facilitation, we used our prior studies to detail a model for group visit structure, e.g., components and timing for breakout sessions [16,17,18,19]. We provided questions for learners to ask patients while waiting for their individual patient encounter; these questions focused on how diabetes affects the entire body, broken down system by system (Appendix 1). We also included the role of other medical and clinical staff, such as nurses or Community Health Workers, who may facilitate the social and education portion of the group visit.
To address group visit patient encounters, we created medication algorithms for low-income settings. Our team utilized current guidelines (i.e., American Diabetes Association) as the framework to create three algorithms for glucose-lowering, anti-hypertensive, and anti-hyperlipidemic medications designated for low-income populations (Fig. 2) [12,13,14,15]. In lieu of listing classes, where the prices of medications may differ, the algorithms named the specific low-cost medication. We also informed clinicians that higher-cost medication availability is individualized (e.g., documentation status, income level) and to alert their clinics to work with patient assistance programs if these medications were required.
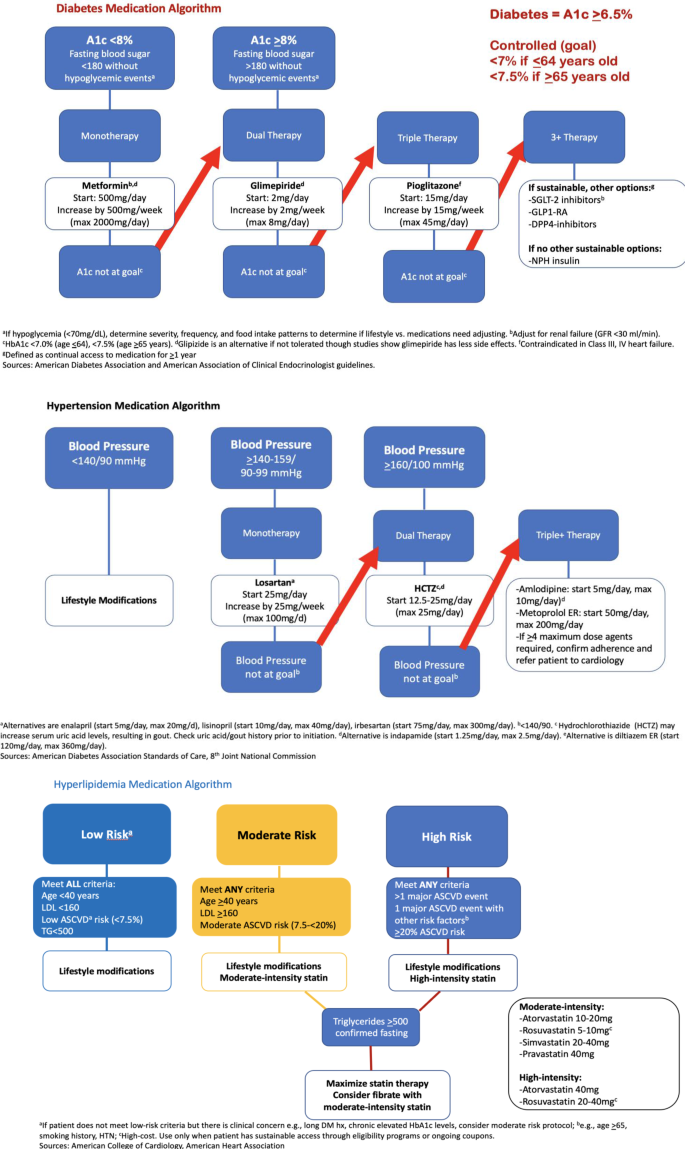
Medication algorithms for diabetes (top), hypertension (middle), and hyperlipidemia (bottom) designed to facilitate sustainable treatment in low-income settings [12,13,14,15]
Implementation step
The Implementation Step consisted of learner instruction and materials. The training was three hours, with the first hour devoted to group visit facilitation, the second hour to patient encounters, and the third hour to addressing questions. Specific components were: icebreaker, introductions, pretest, diabetes and algorithm education, case studies, posttest. Learners were instructed to have their cameras on for the training, and interaction was encouraged throughout the session. We promoted the use of the chat function, text messaging, and a Health Insurance Portability and Accountability Act (HIPAA) secure and encrypted app during the training to increase interaction [20]. We limited training sessions to 10 individuals to enhance learning quality in a virtual setting.
Evaluation step
The Evaluation Step enabled assessment of the course’s success, measured by quantitative (learner recruitment, knowledge change) and qualitative (learner feedback) outcomes. For recruitment, clinic leadership (i.e., medical director) identified interested clinicians. We aimed for the clinic to provide 6–10 individuals to participate in the training for each clinic. For knowledge, we compared pretests and posttests scores. To standardize the training, the tests were identical, ensuring consistent evaluation of learning. The test consisted of 10 questions: 6 multiple choice and 4 fill-in-the blank (Appendix 2). The tests were not reviewed until all individuals completed the posttest. We used t-tests for dichotomous outcomes (correct vs. incorrect) with statistical significance set at p < 0.05. For feedback, facilitators reached out to learners by email after the training to obtain their input. Learners sent their responses to the tests and surveys electronically. Authors (MA, LAJ, KS) categorized the survey responses into themes. Any discrepancies were addressed by a senior author (EMV). We followed up with clinicians who participated in group visits one year after the training to gather input on their experiences. We asked for positive feedback, program suggestions, and any additional comments they wished to provide.
link





