Transitioning to adult care in youth-onset diabetes: a scoping review of socio-ecological factors in youth-onset type 2 diabetes compared to type 1 diabetes | BMC Public Health

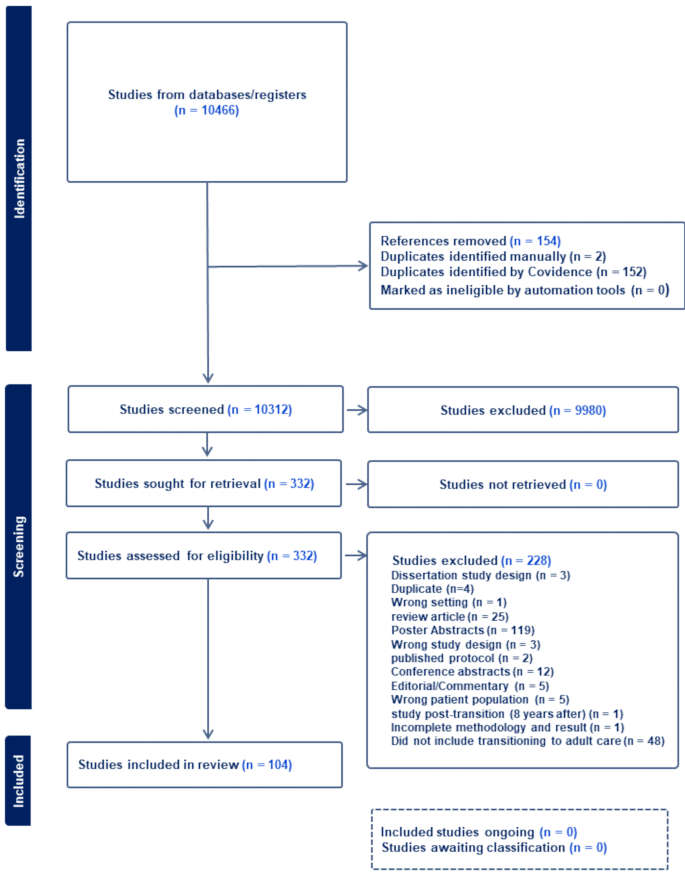
Of the 10,466 articles identified, 332 articles were assessed for eligibility (Fig. 1). Of the 332 articles assessed for eligibility, 25 articles were reviews: two were systemic reviews, and 23 were narrative reviews. Although four of the narrative reviews mentioned Y-T2D in addition to Y-T1D, none of the reviews distinguished between factors influencing transitioning in Y-T1D and Y-T2D [13, 20,21,22]. One hundred and four articles were included in the scoping review, of which three were translated to English [23,24,25]. Only two studies were published before 2000 and the majority of studies that included Y-T2D were published after 2010. Table 1 shows the study design and population demographics of the 104 included studies. Most articles published (88%, n = 91) reported on transitioning of care in Y-T1D, 2% (n = 2) investigated transitioning in a Y-T2D cohort only, 6% (n = 7) compared Y-T1D and Y-T2D populations, and 4% (n = 4) did not specify the diagnosis type (Fig. 2; Table 2). Two-thirds of articles were conducted in a healthcare setting. Table 1 illustrates the study design and demographics grouped by population; 63% percent of studies reported on participants in North America with 52% percent in the United States of America (Table 1, Supplemental Table 1). Many participants were female and white ethnicity (Table 1), but only 43% of studies reported demographic data on race/ethnicity. 50% of studies used quantitative study design. In Y-T1D, there were: two randomized controlled, two non-randomized controlled, ten cohort, seventeen cross-sectional, fifteen longitudinal, thiry-seven qualitative, and eight mixed methods design. In studies that included Y-T2D/ Both: there were no randomized trials, two cohort, one cross-sectional, three longitudinal, three qualitative, and two mixed methods design.
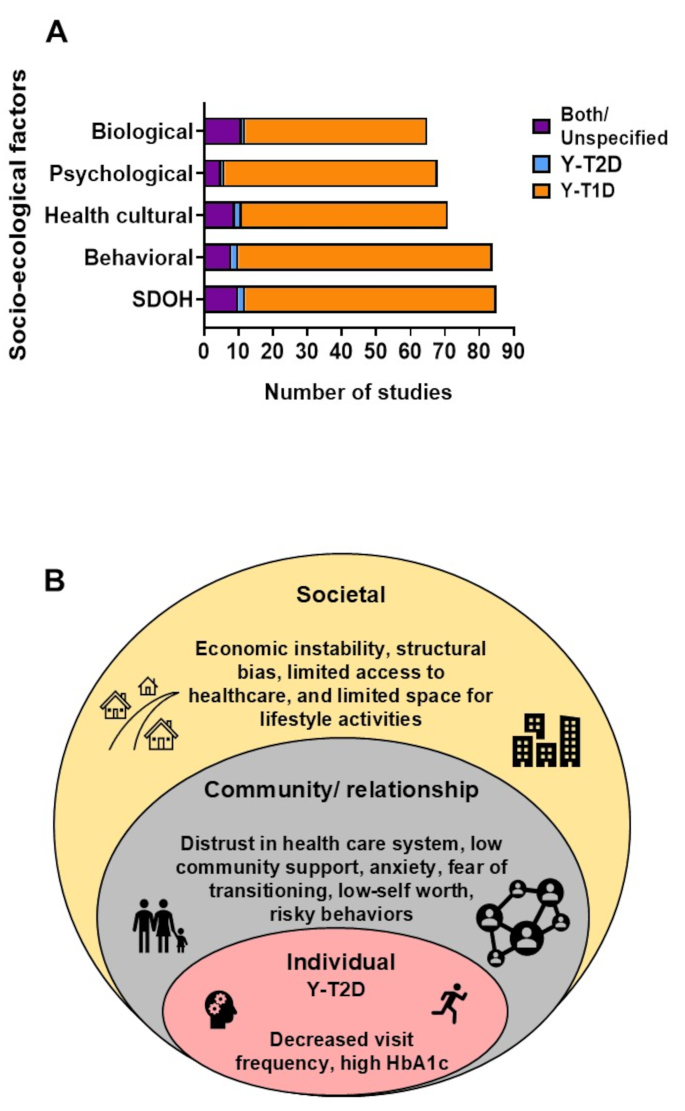
Socio-ecological Factors reported in studies of transitioning to adult diabetes care. (A) Bar graph showing percent of studies that reported social determinants of health (SDOH), health cultural factors, psychological factors, behavioral factors, and biological factors among all by population, Both/ Unspecified youth diabetes (purple), youth-onset type 2 diabetes (blue), and youth-onset type 1 diabetes (orange). (B) Reported barriers to transitioning to adult care conceptualized within the socio-ecological model. The model highlights the interrelationship between each level (circle) [91, 94,95,96, 98, 100]
Transition-related factors characterized by socio-ecological domains of influence
The number of studies categorized by socio-ecological factor collected in Y-T2D and Y-T1D is illustrated in Fig. 2A and reported in Supplemental Table 1.
Societal factors
Most studies (82%) analyzed the association of transition care with social determinants of health (Fig. 2A). Specific factors detailed in the studies differed by population, and there was no universal societal factor collected across all studies. In Y-T1D studies, social determinants of health reported included: access to healthcare [23, 26,27,28,29,30,31,32,33,34,35,36,37,38,39,40,41,42,43,44,45,46,47,48,49,50,51], economic stability [23, 25, 30, 47, 52,53,54,55,56,57,58,59,60,61,62,63,64,65,66,67,68], education and policies [23, 25, 26, 30, 32, 35, 37, 40, 42, 44, 46,47,48, 50, 51, 53, 55,56,57,58,59,60, 62,63,64,65, 68,69,70,71,72,73,74,75,76,77,78,79], neighborhood and built environment [28, 34, 39, 42, 48, 53, 55, 56, 58,59,60, 62,63,64, 69, 70, 74, 79,80,81,82], social and community support [23, 25,26,27,28,29,30, 35, 38, 41, 43, 44, 47, 49, 52,53,54,55, 63,64,65,66,67,68, 70, 71, 73, 74, 77,78,79,80,81,82,83,84,85,86,87,88,89,90], food insecurity [63], and poverty [23, 32, 39, 54, 63]. No studies in Y-T1D investigated structural bias. In Y-T2D/Both studies, two thirds reported on access to healthcare [91,92,93,94,95,96,97,98,99], structural bias [91], poverty [98], education and policy [94, 96], economic stability [91, 94, 96, 98], social and community support [91, 93, 95, 97, 100, 101], and neighborhood and built environment [91, 94, 98]. No articles reported on the impact of food insecurity on transitioning to adult diabetes care in Y-T2D.
Community/ relationship factors
Health cultural
Reporting of health cultural factors was common and collected in 68% of all studies (Fig. 2). Health cultural factors commonly collected in Y-T1D included: attitudes towards health care [26, 27, 30, 34,35,36,37, 39, 45, 47, 51, 55, 56, 59, 61, 63, 68, 72, 73, 77, 79, 82, 83, 87, 102,103,104,105,106], health cultural attitudes [26, 28, 30, 32, 34,35,36, 41, 43, 46, 47, 55, 56, 58, 59, 63,64,65, 68, 73, 81,82,83, 86, 89, 102, 104,105,106,107,108,109], community or provider diabetes care practices [26, 30, 31, 35, 36, 38, 43, 46, 48, 49, 51, 61, 64, 72, 77, 79, 82,83,84, 86, 89, 104,105,106, 108, 110], and multi-disciplinary clinics [39, 45, 64, 73, 83, 86, 104, 106, 108, 110]. Eleven studies reported on at least one health cultural factor in Y-T2D/ Both; attitudes towards health care [91, 93,94,95, 101], health cultural attitudes [91, 93,94,95, 97, 100], community or provider diabetes care practices [93, 95, 97], and multi-disciplinary clinics [93, 95,96,97]. The presence of multi-disciplinary clinic and easy access to adult healthcare provider facilitated transitioning to adult-centered care [91].
Psychological
Data documenting mood symptoms, anxiety or depressive disorders were reported in 59% of all studies (Fig. 2A). In Y-T1D, one study examined the impact of early childhood adversity [84], one on post-traumatic stress disorder [31], and multiple assessed disordered eating behaviors [28, 31, 32, 40, 109,110,111,112,113], depressive symptoms [24, 25, 27, 28, 31, 32, 36, 38, 40, 44, 58, 61, 62, 69, 81, 110,111,112,113,114,115], and anxiety-related symptoms [24, 28, 31, 32, 40, 44, 61, 81, 112, 113, 116]. In Y-T2D, few studies assessed mood symptoms (depression and anxiety [91, 94, 100]) and stress [97]. We did not find any studies that collected data on eating disorders, early childhood adverse events, or post-traumatic stress disorder in Y-T2D.
Behavioral
Eighty-four studies (Fig. 2) collected data on behavioral factors. In Y-T1D, studies included data on self-management and medication adherence support [24, 26,27,28,29, 31, 33,34,35,36, 38, 41,42,43, 46, 47, 52, 53, 56, 57, 59, 62,63,64,65,66,67,68,69,70, 72,73,74, 76, 78,79,80,81, 83,84,85,86,87, 90, 102, 105,106,107,108,109, 111, 116,117,118,119]. Specific behaviors that impeded outcomes included substance abuse, neglect, use of technologies, transition readiness, and medication dosing. Diabetes self-management strategies were reported on a range of activities, including dietary choices, physical activity, blood glucose monitoring, and medication management. Nine Y-T2D/ Both studies reported on behavioral factors including information on scheduling and attending appointments, self-management strategies, blood glucose monitoring, medication management, and goal setting [91, 93, 95,96,97, 100, 101, 120, 121]. Additional behaviors that were found to impede outcomes were social isolation [91], risky behaviors (e.g., substance use, previous incarceration) [120], and lack of chore engagement [101]. We did not find any studies that reported on dietary choices and physical activity in Y-T2D during transition.
Individual/ biological factors
Metabolic biomarkers (body mass index, HBA1c, weight, fructosamine, blood pressure, cholesterol, urine albumin, serum bicarbonate, and ketones) were collected in 58 studies (58% Y-T1D, 50% Y-T2D, 36% of both). No studies examined fasting glucose or fasting insulin concentrations.
Facilitators and barriers to transitioning care in Y-T2D [96]
Figure 2B illustrates cited barriers experienced in Y-T2D/ Both across the socio-ecological domains. Table 2 details the main results for the studies that included Y-T2D by diagnosis grouping. Most studies evaluated the outcomes of transitioning to adult care while only 2 studies assessed the effect of formulated transition programs [101, 122]. The association of transitioning to adult care was inconsistently related to worsening glycemic control and poor outcomes. For example, the transitioning period was related to 4-fold higher odds of HbA1c greater than 9% in Y-T2D in the SEARCH for Diabetes in Youth Cohort [92]. Though, the transition period was not related to increased diabetes-related hospitalizations in the United States [98]. In contrast, a robust prospective cohort study in Canada described higher rates of hospitalizations and fewer medical visits in the transitioning period in Y-T2D compared to Y-T1D [94]. A retrospective analysis from Australia found poor diabetes-related outcomes related to fewer medical visits [120]. Frequent HbA1c testing in Y-T2D was not a predictor of glycemic outcomes or microvascular complications compared to Y-T1D [123].
Feelings of anxiety, depression, and low self-worth were prevalent among transitioning Y-T2D and Y-T1D, although there was a small sample size of Y-T2D in these studies [91, 95, 100]. Y-T2D reported economic challenges, life transition, stigma, a sense of guilt, and fear of being judged by others as impediments to transitioning to adult-centered care [91]. Other factors related to poor diabetes outcomes in Y-T2D were structural bias, poverty, economic instability, access to quality healthcare, neighborhood and built environment, and social and community support [91, 94, 96, 98].
Four studies investigated the factors contributing to resiliency and mitigating strategies Y-T2D/ Both [93, 94, 96, 101]. Routine performance of household chores [101], easy access to clinics located in close proximity to the pediatric clinic, purposeful developmental age-appropriate diabetes education, older age during transfer to adult care [93], an internet-based program [96], the presence of a multi-disciplinary clinic, and easy access to adult healthcare providers [91] were identified facilitators of transition care. Difficulty establishing rapport with patients, abrupt transition to a new clinic, long waiting period for appointments, and relocation to the new environment were barriers to transitioning to adult care [94, 96]. The presence of a multi-disciplinary clinic and easy access to adult healthcare providers facilitated transitioning to adult-centered care [91].
link





